calsfoundation@cals.org
West Nile Virus
West Nile virus (WNV) is an arthropod-borne, positive-sense, single-stranded RNA flavivirus (family Flaviviridae, genus Flavivirus) that has emerged as a significant health risk for humans. WNV is one of several Japanese encephalitis antigenic serocomplex of viruses that also include Japanese encephalitis virus, Murray Valley encephalitis virus, St. Louis encephalitis virus, and some other flaviviruses. West Nile has also been associated with illness and death in a wide variety of North American reptiles, birds, and mammals. It was first recognized in Arkansas in 2002.
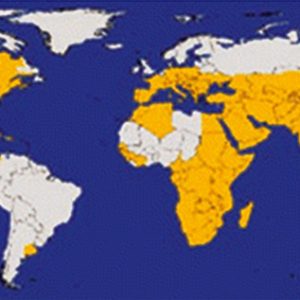
WNV was first identified in 1937 in the West Nile District of the Republic of Uganda of eastern Africa. Prior to 1995, the last major human outbreak of WNV was in the 1950s in Israel. The ecology and epidemiology of WNV started to change in the mid-1990s when an epidemic of human encephalitis occurred in Romania. However, smaller outbreaks in humans and equines had also been identified in other parts of the world in the mid-to-late 1990s: in Morocco (1996), Tunisia (1997), Italy (1998), and Israel (1998). Interestingly, as the later North American outbreak progressed, a similar WNV outbreak was uncovered in Russia at the same time.
The first case of the virus in North America was detected in the New York City area in 1999. Within three years of its initial appearance, WNV activity was reported in the forty-eight states (and Washington DC) that make up the continental United States. The epizootic also expanded to Mexico, the Caribbean, and Central America; it was first recognized in Arkansas in 2002. In the United States alone, more than 30,000 people have been infected with WNV since its arrival in the late 1990s, and thousands of cases are being reported each year, with most occurring in August and September. In addition, serological evidence of exposure to WNV has been reported in many other North American species in which the disease had not been previously recorded. There have been human cases and equine cases, and many birds are infected. The first nonhuman primate to contract WNV was the Barbary macaque, Macaca sylvanus.
Research of phylogenetic lineages has led to the conclusion that WNV emerged as a distinct virus about 1,000 years ago. This original virus developed into two distinct lineages as follows: (1) lineage 1 WNV and its multiple profiles is the source of the epidemic transmission in Africa and throughout the globe, and (2) lineage 2 WNV was regarded as an African zoonosis. However, in 2008, lineage 2 WNV, previously only observed in horses in Madagascar and Sub-Saharan Africa, began to appear in horses in Europe. Here, the first known outbreak affected eighteen animals in Hungary. Lineage 1 WNV was detected in South Africa in 2010 in a mare that had an aborted fetus with the disease; previously, only lineage 2 WNV had been detected in horses and humans in South Africa. Interestingly, a fatal case in 2007 in a killer whale (Orcinus orca) in a marine park in Texas widened the known host range of WNV to include marine mammals, specifically cetaceans.
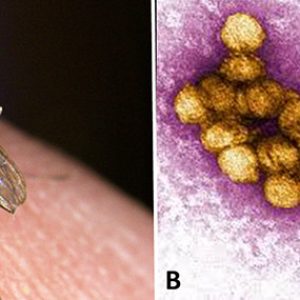
WNV is transmitted by mosquito vectors, primarily Culex spp. It has been demonstrated in a large number of species, but the most significant for viral transmission are several Culex species that feed on birds, including C. erraticus, C. nigripalpus, C. pipiens, C. quinquefasciatus, C. restuans, C. salinarius, and C. tarsalis. Mosquitoes are extremely environmentally tolerant and are nearly cosmopolitan in geographical distribution, being present on all major land masses except Antarctica and Iceland. Nevertheless, climate change and land use on ecological timescales can variously expand or fragment their distribution patterns, raising consequent concerns for human health. Experimental infection has also been demonstrated with argasid (soft) tick vectors, but they are unlikely to be important in natural transmission.
There are several modes of transmission, but the most common source of infection in humans is via a blood meal being taken by an infected mosquito vector. Other modes of transmission include blood transfusion, organ transplantation, breastfeeding, transplacental transmission, and laboratory acquisition. However, these alternative modes of transmission are extremely rare. Unlike in birds, it does not otherwise spread directly between humans.
The primary natural hosts of WNV are birds; therefore, the virus remains within a “bird-mosquito-bird” transmission cycle. While severe clinical disease develops in a minority of humans and horses with WNV infection, the condition in birds appears to be considerably different in North America. Both the Israeli and American strains of WNV are marked by high mortality rates in infected avian populations, as the presence of dead birds, especially American crows, Corvus brachyrhynchos (family Corvidae), can be an early indicator of the arrival of the virus. Illness and death in birds other than crows with WNV, such as Chilean flamingos (Phoenicopterus chilensis) and a snowy owl (Bubo scandiacus), occurred in the Bronx Zoo in New York soon after the initial discovery in the United States. Other North American birds are highly susceptible to this virus.
Over 300 different species of birds have been shown to be infected with the virus. Some birds, including the blue jay (Cyanocitta cristata) and greater sage-grouse (Centrocercus urophasianus), are killed by the infection, but others do survive. The American robin (Turdus migratorius) and house sparrow (Passer domesticus) are thought to be among the most important reservoir species in cities of North America and Europe. Other common North American birds in which high levels of antibodies against WNV have been found are brown thrashers (Toxostoma rufum), gray catbirds (Dumetella carolinensis), northern cardinals (Cardinalis cardinalis), northern mockingbirds (Mimus polyglottos), wood thrushes (Hylocichla mustelina), and those in the dove family, Columbidae. However, the factors that make some species highly susceptible to WNV remain mostly undetermined.
WNV has a broad host range and is also known to be proficient in infecting at least thirty mammalian species, including some non-human primates, horses, cats, and dogs. Some infected humans and horses experience disease, but dogs and cats rarely show symptoms. Mammals are considered incidental or dead-end hosts for the virus, as they do not usually develop a high enough viral load in the blood (viremia) to infect another mosquito feeding on them and carry on the transmission cycle; some birds are also dead-end hosts. Reptiles and amphibians can also be infected, including some species of crocodiles, alligators, snakes, lizards, and frogs.
In the enzootic or normal rural transmission life cycle, the virus alternates between the bird reservoir and the mosquito vector. It can also be transmitted between birds via direct contact, by eating an infected bird carcass, or by contaminated water. In mosquitoes, vertical transmission between female and offspring is possible, and might potentially be important in being able to survive overwintering. In the spillover or urban cycle, infected mosquitoes that have fed on infected birds transmit the virus to humans. These are termed bridge vectors, that is, mosquito species that bite both birds and humans.
All age groups of humans are equally likely to be infected, but there is a higher amount of death and neuroinvasive WNV in people between the ages of 60 and 89. WNV can cause a disease known as West Nile fever. Elderly people are more likely to have adverse effects of being infected. Those human hosts infected by WNV develop symptoms typically within three days to two weeks after they are bitten by an infected mosquito. Many people are bitten by mosquitoes that harbor WNV, but most do not realize they have been exposed. Main risk factors for severe disease include: (1) age over 50 to 60 with other health problems, and (2) conditions that weaken the immune system, such as HIV/AIDS, organ transplants, and recent chemotherapy.
Historically, people who reside or frequent areas where the virus was endemic, such as the Nile Delta of Egypt southward, usually experienced subclinical or mild disease. Furthermore, not all people show symptoms, in fact, the majority (80 percent) have few or no symptoms. About 20 percent of people develop mild symptoms such as fever, headache, body aches, nausea, vomiting, and sometimes swollen lymph glands or a skin rash on the chest, stomach, and back; their symptoms can last for only a few days, though even healthy people have become ill for several weeks. Less than one percent of patients develop severe symptoms, such as meningoencephalitis with a collection of associated physical problems including high fever, headache, neck stiffness, stupor, disorientation, coma, tremors, convulsions, muscle weakness, vision loss, numbness, and paralysis. These symptoms may last several weeks, and neurological effects may be permanent. Recovery may take weeks to months, and the risk of death among those in whom the central nervous system is affected is about ten percent. Almost 13,000 of the individuals who reported as having WNV between 1999 and 2019 were seriously ill, and more than 1,200 died.
Infection with WNV appears to be seasonal in temperate zones. In those, such as in the United States and Europe, peak season is from July to October. Depending on geographic region, peak season can change, particularly in warmer and humid climates that can experience longer peak seasons. Furthermore, higher ambient temperatures in winter months and warmer spring may lead to larger summer mosquito populations, increasing the risk for WNV. Similarly, increased precipitation may also further mosquito reproductive rates and affect the seasonality and geographic variations of the virus. For example, studies have shown an association between heavy precipitation and higher incidence of documented WNV. Likewise, high winds can serve as another environmental factor that functions as a dispersal mechanism for mosquito vectors.
WNV affects horses far more than any other animal, except humans. Between 1999 and 2019, more than 25,000 cases of WNV encephalitis were reported in U.S. horses. In equine hosts, severe disease may or may not occur. The most common signs of WNV infection in horses include stumbling, incoordination, weak limbs, partial paralysis, and muscle twitching. It is also reported that the residual effects of gait and behavioral abnormalities can persist in approximately 40 percent of affected horses for up to six months following infection. However, those with severe neurologic effects might not regain the ability to stand and might experience convulsions and/or blindness, and so are usually humanely euthanized. A veterinary vaccine for horses has become available and is 100 percent effective. However, before the availability of vaccines, around 40 percent of horses infected in North America died.
In amphibians, experimental infection of the marsh frog (Rana ridibunda) with a Russian strain of WNV resulted in high levels of viremia. In reptiles, WNV has been reported in Nile crocodiles (Crocodylus niloticus), and there have been epizootic outbreaks in farmed alligators (Alligator mississippiensis), with the virus causing various pathologies, including heterophilic granulomas, heterophilic perivasculitis, multiorgan necrosis, and lymphoplasmacytic meningoencephalitis. In addition, one captive Salvador’s monitor (Varanus salvadorii) with neurologic signs of WNV has been reported, as well as a Caspian turtle (Clemmys caspica) that was found to be seropositive for WNV. Very high viremia titers have been reported in various reptiles, suggesting that they could play a role as an amplification host. However, the role of amphibians and reptiles in the life cycle and epidemiology of WNV remains unknown.
In humans, laboratory diagnosis is typically based on overt symptoms and positive blood tests of serum showing a rising level of antibodies. Spinal taps are occasionally done for testing cerebrospinal fluid (CSF) attempting to detect or rule out WNV-specific IgM antibodies. Other tests include electroencephalography (EEG) or an MRI scan that can help detect brain inflammation. In addition, viral cultures and tests (RT-PCR) to detect viral RNA can be performed on serum, CSF, and from tissue specimens that are collected early in the course of the disease and, if results are positive, can confirm an infection. Immunohistochemistry (IHC) can detect WNV antigen in formalin-fixed tissue. However, negative results of these tests do not rule out WNV infection. While there are no specific treatments, pain medications may be useful. There is no human vaccine, but efforts have been made to produce a vaccine for human use; several candidates have been produced, but by 2021, none were yet licensed for usage.
Preventative efforts against WNV focuses mainly on avoidance of human contact with and being bitten by infected mosquitoes. When in an area that has WNV, it is important that individuals limit or outright avoid outdoor activity and, when they do go outside, use a mosquito repellent containing N, N-diethyl-meta-toluamide (DEET), picaridin, oil of lemon eucalyptus (OLE), or IR 3535 (SkinSmart). Eliminating standing pools of water, such as in buckets, gutters, old tires, and swimming pools, is helpful. It is also recommended to drain or treat standing water around homes with a mosquito larvicide to reduce mosquito breeding sites. For example, exposure of mosquito larvae to Bacillus species, specifically Bacillus thuringiensis israelensis, results in larvae having difficulty digesting food they eat after the exposure; they then die of starvation.
Using mosquito netting and avoiding areas where mosquitoes occur may also be useful. A person can also wear clothing that covers more of the body, such as long sleeves and pants. Mosquito control can also be done at the community level and include surveillance programs and control programs including pesticides and reducing mosquito habitats. A good example of this program is done each mosquito season in Jonesboro (Craighead County). Surveillance systems regarding birds are particularly useful. If dead birds are found in a neighborhood, it should be reported to local authorities. This may help health departments determine if the birds are infected with WNV.
The number of WNV cases rose across the United States in 2018, with 167 people dying from the disease. According to WNV statistics kept by the Arkansas Department of Health in Little Rock (Pulaski County) since 2011, by 2019, 156 people had died in the state from WNV, with the most cases (64) in 2012. In 2018, the five leading states with the most cases of WNV included: South Dakota (40 cases), Louisiana (25 cases), Mississippi (23 cases), California (21 cases), and Texas (17 cases). In 2024, Arkansas reported 13 cases of West Nile Virus.
For additional information:
Ariel, Ellen. “Viruses in Reptiles.” Veterinary Research 42 (2011): 42‒100.
Bolling, B. G., J. H. Kennedy, and Earl G. Zimmerman. “Seasonal Dynamics of Four Potential West Nile Vector Species in North-Central Texas.” Journal of Vector Ecology 30 (2005): 186‒194.
Brinton, Margo A. “The Molecular Biology of West Nile Virus: A New Invader of the Western Hemisphere.” Annual Review of Microbiology 56 (2002): 371–402.
Bugbee, L. M., and L. R. Forte. “The Discovery of West Nile Virus in Overwintering Culex pipiens (Diptera: Culicidae) Mosquitoes in Lehigh County, Pennsylvania.” Journal of the American Mosquito Control Association 20 (2004): 326–327.
Colpitts, Tonya M., Michael J. Conway, Ruth R. Montgomery, and Erol Fikrig. “West Nile Virus: Biology, Transmission, and Human Infection.” Clinical Microbiology Reviews 25 (2012): 635–648.
Dahlina, C. R., D. F. Hughes, Walter E. Meshaka Jr., C. Coleman, and J. D. Henning. “Wild Snakes Harbor West Nile Virus.” One Health 2 (2016): 136–138.
Eidson, M., N. Komar, F. Sorhage, R. Nelson, T. Talbot, and F. Mostashari. “West Nile Virus Avian Mortality Surveillance Group. Crow Deaths as a Sentinel Surveillance System for West Nile Virus in the Northeastern United States, 1999.” Emerging Infectious Diseases 7 (2001): 615–620.
Gamino, Virginia, and Ursula Höfle. “Pathology and Tissue Tropism of Natural West Nile Virus Infection in Birds: A Review.” Veterinary Research 44 (2013): 39.
Kilpatrick, A. M., S. L. LaDeau, and P. P. Marra. “Ecology of West Nile Virus Transmission and Its Impact on Birds in the Western Hemisphere.” The Auk 124 (2007): 1121–1136.
Komar, N., J. Burns, C. Dean, N. A. Panella, S. Dusza, and B. Cherry. “Serologic Evidence for West Nile Virus Infection in Birds in Staten Island, New York, after an Outbreak in 2000.” Vector Borne Zoonotic Diseases 1 (2001): 191–196.
Komar, N., N. A. Panella, J. E. Burns, S. W. Dusza, T. M. Mascarenhas, and T. O. Talbot. “Serologic Evidence for West Nile Virus Infection in Birds in the New York City Vicinity during an Outbreak in 1999.” Emerging Infectious Diseases 7 (2001): 621–625.
Lanciotti, R. S., G. D. Ebel, and V. Deubel, et al. “Complete Genome Sequences and Phylogenetic Analysis of West Nile Virus Strains Isolated from the United States, Europe, and the Middle East.” Virology 298 (2002): 96–105.
Lanciotti, R. S., A. J. Kerst, R. S. Nasci, M. S. Godsey, C. J. Mitchell, and H. M. Savage. “Rapid Detection of West Nile Virus from Human Clinical Specimens, Field-Collected Mosquitoes, and Avian Samples by a TaqMan Reverse Transcriptase-PCR assay.” Journal of Clinical Microbiology 38 (2000): 4066–4071.
Lawrie, Charles, Nathalie Uzcátegui, Ernest Gould, and Patricia Nuttall. “Ixodid and Argasid Tick Species and West Nile Virus.” Emerging Infectious Diseases 10 (2004): 653–657.
Londono-Renteria, Berlin, and Tonya M. Colpitts. “A Brief Review of West Nile Virus Biology.” Methods in Molecular Biology 1435 (2016): 1–13.
Mackenzie, John S., Duane J. Gubler, and Lyle R. Petersen. “Emerging Flaviviruses: The Spread and Resurgence of Japanese Encephalitis, West Nile and Dengue Viruses.” Nature Medicine 10 (2004): S98‒S109.
Miller, D. L., M. J. Mauel, C. Baldwin, G. Burtle, D. Ingram, and M. E. Hines. “West Nile Virus in Farmed Alligators.” Emerging Infectious Diseases 9 (2003): 794–799.
Petersen, L. R., and A. A. Marfin. “West Nile Virus: A Primer for the Clinician.” Annals of Internal Medicine 137 (2002): 173–179.
Ratterree, Marion S., Amelia P. A. Travassos da Rosa, Rudolf P. Bohm Jr., Frank B. Cogswell, Kathrine M. Phillippi, Kevin Caillouet, Shelle Schwanberger, Robert E. Shope, and Robert B. Tesh. “West Nile Virus Infection in Nonhuman Primate Breeding Colony, Concurrent with Human Epidemic, Southern Louisiana.” Emerging Infectious Diseases 9 (2003): 1388–1394.
Roehrig, John T. “West Nile Virus in the United States-A Historical Perspective.” Viruses 5 (2013): 3088‒3108.
Sardelis, M. R., M. J. Turell, D. J. Dohm, and M. L. O’Guinn. “Vector Competence of Selected North American Culex and Coquillettidia for West Nile Virus.” Emerging Infectious Diseases 7 (2001): 1018–1022.
Smithburn, K. C., T. P. Hughes, A. W. Burke, and J. H. Paul. “A Neurotropic Virus Isolated from the Blood of a Native of Uganda.” American Journal of Tropical Medicine 20 (1940): 471–492.
Sota, T., E. Hayamizu, and M. Mogi. “Distribution of Biting Culex tritaeniorhynchus (Diptera: Culicidae) among Pigs: Effects of Host Size and Behavior.” Journal of Medical Entomology 28 (1991): 428–433.
St. Leger, J., G. Wu, M. Anderson, L. Dalton, E. Nilson, and D. Wang. “West Nile Virus Infection in Killer Whale, Texas, USA, 2007.” Emerging Infectious Diseases 17 (2011): 1531–1533.
Steinman, Amir, Caroline Banet-Noach, and Shlomit Tal, Ohad Levi, Lubov Simanov, Shimon Perk, Mertyn Malkinson, and Nahum Shpigel. “West Nile Virus Infection in Crocodiles.” Emerging Infectious Diseases 9 (2003): 887–889.
Suthar, Mehul S., Michael S. Diamond Jr., and Michael Gale. “West Nile Virus Infection and Immunity.” Nature Reviews Microbiology 11 (2013): 115–128.
Trock, S. C., B. J. Meade, A. L. Glaser, E. N. Ostlund, R. S. Lanciotti, and B. C. Cropp. “West Nile Virus Outbreak among Horses in New York State, 1999 and 2000.” Emerging Infectious Diseases 7 (2001): 745–747.
Venter, M., S. Human, S. van Niekerk, J. Williams, C. van Eeden, and F. Freeman. “Fatal Neurologic Disease and Abortion in Mare Infected With Lineage 1 West Nile Virus, South Africa.” Emerging Infectious Diseases 17 (2011): 1534–1536.
Chris T. McAllister
Eastern Oklahoma State College




Comments
No comments on this entry yet.